Meduit’s family of web bots solves specific task problems for the hospital revenue cycle.

COVID-19 has inadvertently set the table for AI to transform the revenue cycle. It’s a game-changing tool for hospital RCM, and CEOs are asking for AI solutions and the benefits they bring to the RCM process. These include generating more cash faster, reducing human touches, increasing efficiencies and lowering costs.
| “AI is a game-changer that will deliver month after month after month.” |
Introducing SARA
Meduit leads the industry with innovative solutions under the MeduitAI umbrella that leverage AI and incorporate robotic process automation (RPA) to maximize the revenue cycle. SARA – short for Supervised Autonomous Revenue Associate – is Meduit’s family of web bots that are designed to solve specific revenue cycle tasks.
| “This bot is doing the work of 12 full-time employees for the provider.” |
Applying AI: A North Carolina Blues Case Study
The Challenge: Blue Cross Blue Shield (BCBS) of North Carolina provides actionable information using a set of proprietary reason codes that are not available in a standard ANSI 277 message. A large provider client needed an efficient process to retrieve this granular status of claims from the Blue Cross website and report that status with any relevant notes back to the patient’s electronic file.
The Solution: Meduit developed an autonomous web bot in the SARA family that performs this task. It reads everything it needs from the provider’s patient accounting system, parses the claim, accesses the payer website to retrieve the information and formats the findings into an easy-to-read note that is posted directly back into the provider’s patient accounting system. Claim rejections and error details are documented in the notes. The solution handles complex searches including out-of-state Blue Cross plans. No IT integration was required by the provider to implement this solution, so it was zero upfront investment cost. The provider simply provided a set of remote access user credentials and BCBS NC credentials.
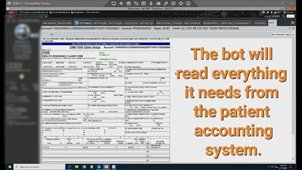
The bot will read everything it needs from the patient accounting system.
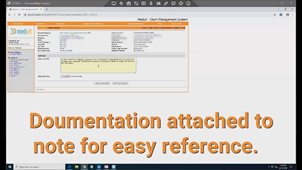
The bot captures substantiation for all claim statuses.
“This bot is doing the work of 12 full-time employees for the provider,” said Jason Petrasich, Meduit’s Senior Vice President of AI, who leads development of the SARA family of bots for Meduit. “For providers who are challenged to find experienced, qualified employees to support their revenue cycle operation, AI is a game-changer that will deliver month after month after month.”
Areas where MeduitAI is already impacting RCM include:
- Clinical coding
- Pre-authorization
- Claims follow-up
- Predicting patient and payer actions
AI Solutions Augment Staff Efforts
The best and most effective AI solutions are meant to work hand-in-hand with staff to get tasks completed more efficiently and accurately, freeing staff to pivot their time to other, higher complexity needs.
“It’s important to remember that AI is not designed to eliminate jobs, but to transform what people do today and how to make the entire process more efficient,” said Petrasich. “AI will remodel the nature of the healthcare workforce.”